Hand injuries provide a distinct set of problems. Hand injuries may be highly inconvenient, in addition to the discomfort they cause. There are easy actions you may do to hasten your recovery while minimizing pain.
Exercises for the Hands
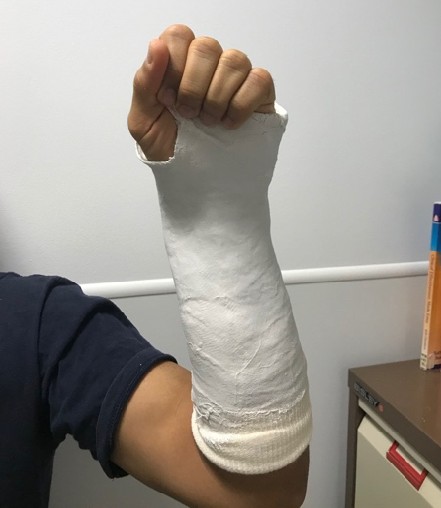
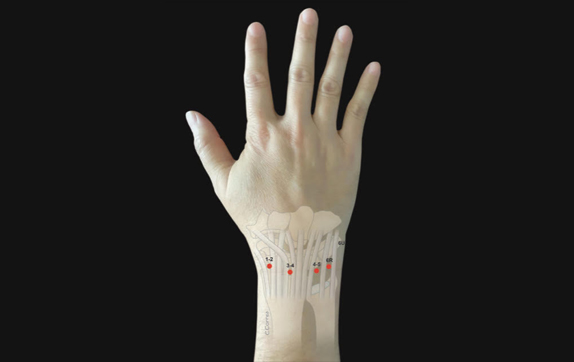
First it is extremely important to ensure that there is no underlying fracture (broken bone), joint dislocations, nerve or tendon injury before commencing any exercises. Early identification and correct treatment at the right time be it splinting, guided hand therapy or surgery if necessary can ensure optimal outcomes.
Speaking with your hand surgeon or hand therapist to identify the best physical therapy program is critical for people with unique hand problems. Depending on your specific injury, one or more of these hand exercises may be required for a speedy recovery.
Delayed identification of more serious problems in these seemingly minor injuries can often lead to adverse outcomes that may significantly affect the function of your hand.
Whether you’re a student-athlete, an office worker with carpal tunnel syndrome, or someone who has recently been diagnosed with arthritis, one of these exercises might help you get back on your feet. The workouts mentioned below are some of the most often suggested. These are also excellent exercises for anyone wanting to increase their hand mobility in general.
Again if you are in pain or have a swollen, or recently injured hand please consult a hand specialist before commencing any of the exercises below.
- It’s as easy as it sounds to make a fist. Begin with your hand spread out in front of you, then create a fist.
- Stretch your fingers by starting with your hand in a natural posture on a flat surface and gradually straightening them. Hold this stance for roughly a minute before switching hands.
- Place your palm flat on the table and slowly raise each individual finger to increase your flexibility. For each hand, repeat this exercise 8-12 times.
- Stretch each of your fingers to contact your thumb while holding your hand in an upright posture.
- For 30-60 seconds, move your fingers into a claw-like stance with your palm facing out.
- With each hand, squeeze a grip-strengthening ball as tightly as possible 10-15 times.
- Pinch a soft foam ball between the tips of one of your fingers and your thumb to strengthen your grip. Do this for approximately a minute, then do it again for a total of 10-15 times.
- Elevate your wrist by draping it over the edge of a folded towel or other similar-sized items. Move your hand up and down completely, starting with your palm facing down and ending with your palm facing up.
- Place your wrist/forearm on a folded-up towel, this time with your hand sideways and your thumb pointing up, like in the last exercise. Then, in a complete range of motion, wave your hand up and down.
- Rotate your arms by placing your palms up, then down, and so on while standing or sitting with your elbows bent at a 90-degree angle.
- Extend your thumb from its natural position to the palm’s center and back.
- Tendon Gliding is an activity that involves placing your hand in various postures and then returning it to a flat position. Make a hook fist first, then a full fist, and finally a straight fist.
Speak with a fellowship-trained Hand Surgeon who specializes in this area right now.
You can traverse the healing phase of your hand injury with relative ease if you follow the advice of a hand surgeon. He/She can assist you in overcoming these obstacles and moving toward long-term recovery. For additional information on how we can help you recover, please contact us.