Your hands are essential instruments for interacting with the outside world. Household duties, work, hobbies, and athletics may all become more difficult if you are unable to use your fingers and hands properly.
Stiffness in the fingers can be caused by a variety of factors, including:
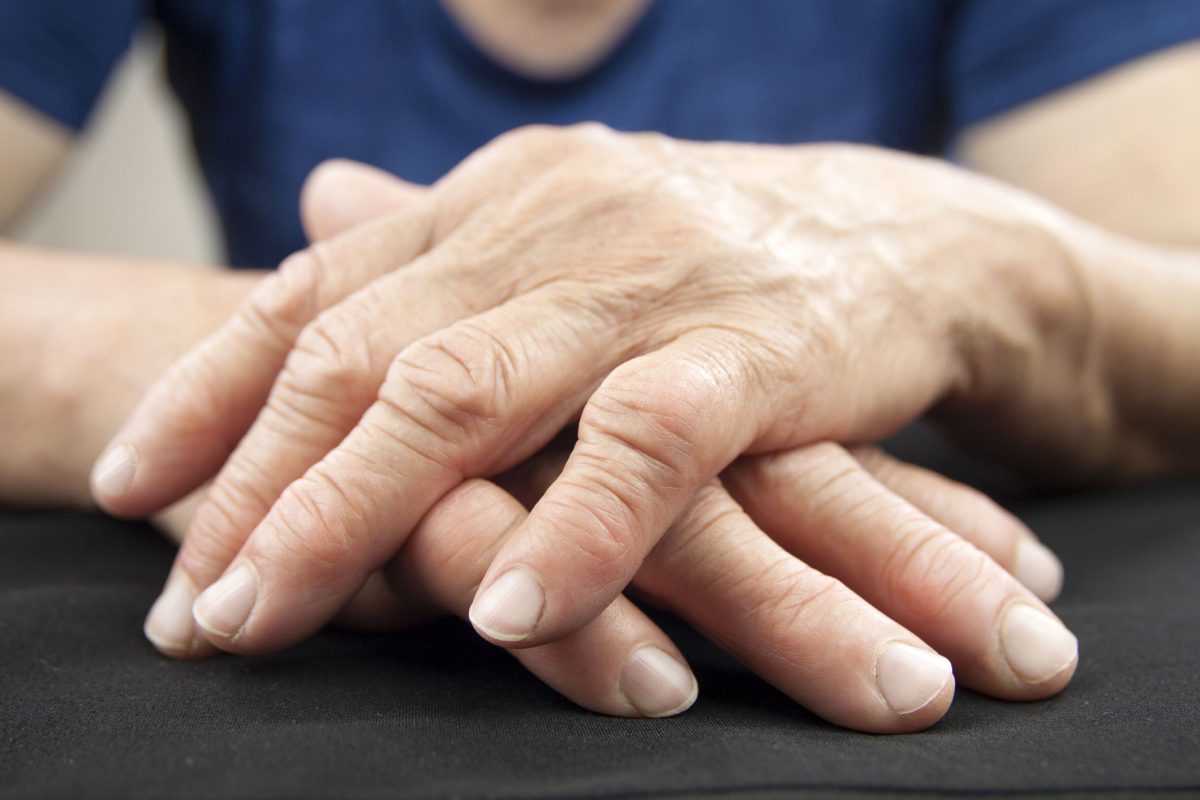
Arthritis
Arthritis comes in various forms, and any of them might induce finger stiffness. Arthritis may be secondary to inflammatory conditions like Rheumatoid arthritis psoriatic arthritis or secondary to trauma or age related degenerative changes. When a joint’s natural smooth gliding is lost, mobility is generally restricted and this can become painful. Depending on the kind of arthritis, the bones in the hand which are most typically afflicted differ. For example psoriatic arthritis affects the end joints of the fingers next to the nail, rheumatoid arthritis has a higher tendency to affect the bigger knuckle joints first. Osteoarthritis ( degenerative) can affect all the 3 joints in the finger. There are staged treatment options available for stiff painful digits starting with medical management, hand therapy and splinting stepping up to surgical intervention if needed.
Injuries
Many of the components of a finger might become stiff if they are damaged.
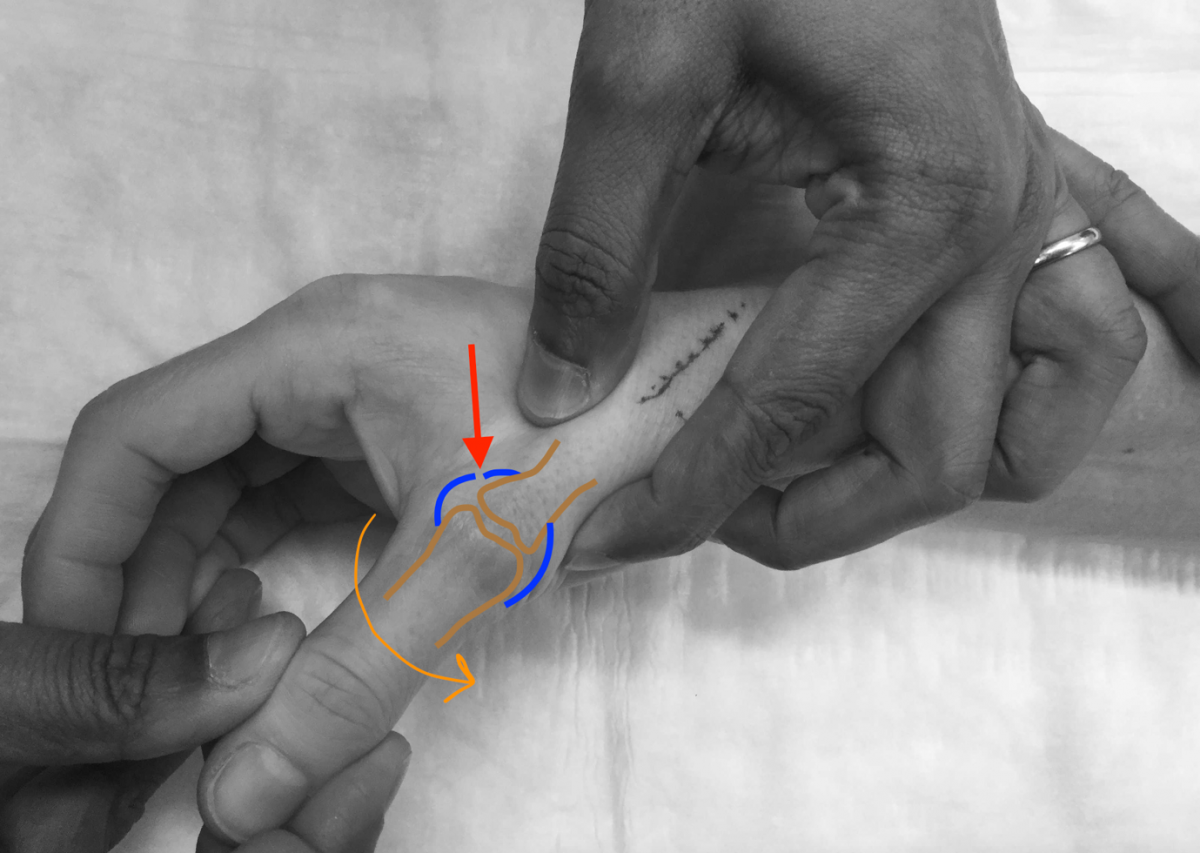
Inflammation of or injury to the tendons around the joint are caused by finger joints dislocations and “jammed fingers.” These injuries can induce permanent or even permanent alterations in the supporting ligaments’ typical flexibility, limiting joint mobility.
Swelling and bleeding from broken fingers (fractures) may be irritant to the tendons that run along the bones. The sharp edges of the broken bone can sometimes injure the tendons. This may cause the tendons to scar to the bone, restricting their mobility and so affecting the joints that those tendons move.
Extensor tendons (straightening) and flexor tendons (bending) injuries in the finger might reduce their range of motion. The tendons’ control joints may lose motion or become stiff as a result.
Temporary plaster slabs/ casts or thermoplastic splints, early hand therapy and range of movement and in certain situations surgery to fix the fracture can help treat the injury.
Normally, the tendons that flex (flex) the fingers glide effortlessly in the tunnels through which they run. When the tendons develop a fullness or lump, they are unable to glide freely in the tunnel. The irregular mobility of the tendon may impede both bending and straightening (like a rope with a knot trying to move through a pulley). These can be treated with early splinting, hand therapy stepping up to steroid injections and in recalcitrant cases surgical intervention
Tendonitis is an inflammation of the tendons (tenosynovitis)
The smooth lining of the tendon (tenosynovium) can swell, restricting their mobility and consequently the movement of the joints they govern. This is particularly problematic when the tendons run through narrow passageways in the hands or wrist. Osteoarthritis, psoriatic arthritis, and trauma or overuse is among conditions that can cause tenosynovium swelling. These too can be treated with early splinting, hand therapy stepping up to steroid injections and in specific cases surgical intervention
Immobilization
Splinting, casting, or bracing are sometimes used to treat finger injuries or surgery. Finger immobilisation for prolonged periods can cause changes in the tissues of the hand (skin, joint linings, ligaments), leading to thickening and scarring and loss of normal flexibility. Seeing the specialist hand therapist and having a clear treatment regime with early mobilisation avoids this.
Burns
Burns can harm not just the epidermis, but also the deeper tissues of the body. Damage secondary to deep scarring frequently causes alterations that result in stiffness.
Complex Regional Pain Syndrome (CRPS)
Complex Regional Agony Syndrome (CRPS) is a disorder characterised by swelling of the hand and fingers, as well as pain. Because of the increased discomfort, the combination causes not only alterations in the tissues that cause stiffness, but also a dread of moving the afflicted portions. This is a very difficult problem to treat and may need multidisciplinary input from hand therapists, pain management consultants and hand surgeons.
Diabetic Stiff hand syndrome
Scientists are still unsure why diabetes increases the risk for hand complications. Possible theories for this condition appear to be related to problems with your body’s collagen. Collagen is a protein that makes up tendons, joints, ligaments and other connective tissue in the body. Increased collagen production, decreased collagen break down, and changes to the composition of collagen can lead to abnormal gathering of proteins in your hands, which makes them more stiff.
It is a condition that affects adults where fibrous bands grow in and beneath the skin as a result of this condition. The capacity to straighten the hands or thumb is usually hampered as a result of these alterations.
Scars
They can occur as a result of any type of injury or surgery. Finger stiffness can be caused by scarring of the epidermis or deeper tissues.
What are the options for treating tight fingers?
The reason of stiff fingers must be determined before the appropriate treatment can be decided. Hand surgeons are well-qualified to determine the cause of your tight fingers. Splinting, casting, bracing, medicines, surgery, and/or hand rehabilitation are some of the options for treatment.
To identify the next stages in your treatment plan, book in for a consultation.